As March marks endometriosis awareness month, we’re delving into the science of ‘endo’, as it’s commonly known, to dissect the science around whether this painful and distressing condition negatively impacts the skin. Dr Scott Ellis, our Clinical Director, breaks down the science of whether acne is a symptom of endometriosis, or if endometriosis causes acne.
What is Endometriosis?
Endometriosis is a condition where cells that normally line the uterus seed into other parts of the body. These cells settle in an area outside of the uterus (most commonly the pelvis) and develop a blood supply that provides them with oxygen, nutrients, and everything else they need to survive. Their presence outside of the uterus creates inflammation which, in some women, leads to chronic pain, heavy periods, scarring and fertility issues. And for anyone that has suffered with this, you will understand just how debilitating endo can be.
Globally, about 10 per cent of reproductive-age women have endometriosis. We don’t really understand why endometriosis happens, except that there appears to be a genetic predisposition (there is a six-fold risk in people with an affected first-degree relative). Generally, endometriosis is treated with hormonal contraceptives, anti-inflammatories, hormone modulating medications or surgery, and it can be a long treatment road for endo sufferers.
How Does Endometriosis Affect The Skin?
Interestingly, we don’t really know if endometriosis affects the skin. Several studies have identified correlations between endometriosis and certain skin conditions, but it seems unlikely that endometriosis is causing these skin conditions to occur.
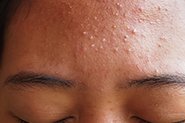
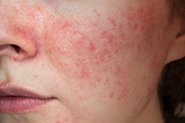
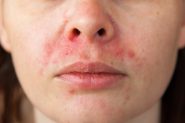
The most discussed correlation is the increased occurrence of acne in those with endometriosis. More specifically, there is a higher rate of severe acne during teenage years in those who have endometriosis either at the time or diagnosed later in life. All too commonly this observation is summarised by statements such as ‘hormonal imbalances in endometriosis drive acne’ – but the science and processes involved in endometriosis say otherwise.
Let’s take an (unapologetically!) deeper dive into the science around this…
Acne is specifically driven by androgens (male sex hormones) that encourage overproduction of skin oil (sebum), drive cell overproduction in hair follicles and help set up the conditions for pimple formation. Endometriosis doesn’t increase the levels of circulating androgens, and as such shouldn’t drive acne in this way. There is a theory that oestrogen and/or progesterone (the female sex hormones) may contribute to acne in mechanisms that we don’t understand. This theory falls over, however, as the introduction of these hormones in the form of the oral contraceptive pill clearly improves acne (and is one of the most common forms of management). Additionally, not all types of endometriosis increase the circulating oestrogen in the body – making this an unlikely explanation.
More recent evidence offers an alternative explanation – that certain genes coding for both endometriosis and acne are actually neighbours, situated extremely close to each other on the same chromosome (chromosome 8q24, for our fellow super-nerds!). As such, a tiny variation in a person’s DNA in one gene is likely accompanied by a variation in the closely located gene – a correlation referred to by geneticists as a ‘linkage disequilibrium’.
Xie et al. (2014) [Reference 7] produced a landmark study that demonstrated the correlation between acne and endometriosis and subsequently suggested this genetic process to be the most likely reason that there is a high rate of acne in those with endometriosis.
Plain Language Summary:
The science suggests that endometriosis doesn’t cause acne (or vice versa), but rather are likely to coexist in a person because their genetic makeup predisposes them to both.
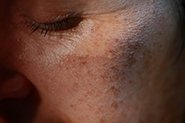
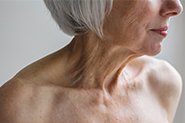
A positive relationship has also been observed between endometriosis and sensitivity to sun exposure, number of freckles, number of nevi (moles), and an increased risk of melanoma (though evidence for the latter is weak). Again, it’s unlikely that endometriosis is the cause of these – rather, it’s more likely that there are similar genetic factors at play.
So, What Does This Mean In The Real World?
Ultimately, those of us who have endometriosis are more likely to struggle with acne (sorry to be the bearer of bad news). But unlike some other gynaecological conditions (such as polycystic ovarian syndrome), treating endometriosis won’t help improve acne. The good news though is that it is possible to treat acne with evidence-based acne treatments to help get your skin under control and keep it happy & healthy.
Our Qr8 MediSkin Medical and Support Teams are experienced in treating adult female acne.
CLICK HERE to see the kind of results we can achieve (and listen to one of our lovely patients chat about her acne journey!) or read more about how we treat acne HERE.
REFERENCES
- Farland LV, Lorrain S, et al. Endometriosis and the risk of skin cancer: a prospective cohort study. Cancer Causes Control. 2017. PMID: 28799019
- Kvaskoff M, Han J, et al. Pigmentary traits, family history of melanoma and the risk of endometriosis: a cohort study of US women. Int J Epidemiol. 2014. PMID: 24343850
- Kvaskoff M, Mesrine S, et al. Personal history of endometriosis and risk of cutaneous melanoma in a large prospective cohort of French women. Arch Intern Med. 2007. PMID: 17954799
- Somigliana E, Viganò P, et al. Association between endometriosis and cancer: a comprehensive review and a critical analysis of clinical and epidemiological evidence. Gynecol Oncol. 2006. PMID: 16473398
- Teal S, Edelman A. Contraception Selection, Effectiveness, and Adverse Effects: A Review. JAMA. 2021. PMID: 34962522
- Brown J, Kives S, Akhtar M. Progestagens and anti-progestagens for pain associated with endometriosis. Cochrane Database Syst Rev. 2012. PMID: 22419284
- Xie J, Kvaskoff M, et al. Severe teenage acne and risk of endometriosis. Hum Reprod. 2014. PMID: 25139175
- Somigliana E, Viganò P, et al. ‘Here comes the sun’: pigmentary traits and sun habits in women with endometriosis. Human reproduction. 2010. PMID: 20083484
- Hu T, Wei Z, et al. Sex hormones and acne: State of the art. J Dtsch Dermatol Ges. 2021. PMID: 33576151
- Clayton RW, Langan EA, et al. Neuroendocrinology and neurobiology of sebaceous glands. Biol Rev Camb Philos Soc. 2020. PMID: 3197085
WOULD YOU LIKE TO CHAT TO ONE OF OUR FRIENDLY DOCTORS ABOUT YOUR SKIN?
CLICK HERE TO BOOK A CONSULT WITH OUR EXPERIENCED MEDICAL TEAM.