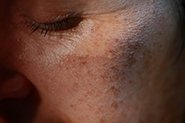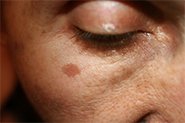
Qr8’s Founder, Dr Michele Squire, is here to explain more about sun protection and Melasma.
Melasma is a frustrating and emotionally distressing skin condition that causes brown or grey-brown patches to appear on the face, particularly on the cheeks, nose, forehead, chin, and upper lip. Unfortunately, melasma is considered a chronic skin disorder, and there is no known cure.
Treating it can be a challenge, as over-the-counter fading products are generally ineffective (including fan favourite, Vitamin C!), microneedling is not an evidence-based treatment for this type of pigment, and many laser and light-based treatments, and peels, may initially fade the pigment only for it to come back darker than before.
However, there is hope for those suffering from melasma! At Qr8, we successfully treat many patients with melasma, helping to both fade pigmentation and minimize its return in the long term. Our topical treatment creams are considered the gold standard for melasma treatment in the scientific literature.
But getting a science-backed fading treatment is only half the story! After treating thousands of patients with melasma, we know the single most critical factor for treatment success and maintaining results is proper sun protection, and using evidence-based sunscreens that are known to help in melasma. This is because melasma pigment is exquisitely sensitive to both visible light and UV radiation from the sun.
What are the types of UV radiation and how do they affect the skin?
There are three types of UV rays: UVC, UVA, and UVB. We don’t need to pay much attention to UVC rays as they are blocked by the atmosphere and don’t make it to the earth’s surface. UVA rays make up 95% of the UV radiation that reaches the earth’s surface. They penetrate deep into the lower layers of skin (the dermis) and are mostly responsible for the formation of free radicals and collagen breakdown that leads to skin aging. These rays are particularly troublesome as they don’t produce any burning or heat and vary only slightly in winter, meaning your skin is exposed to them all year round without you knowing. To make matters worse, they also penetrate through glass, so your office windows and your car’s windscreen offer little protection.
UVB rays make up the remaining UV radiation reaching the earth, and they are responsible for sunburn (‘B’ for ‘burning’, ‘A’ for ‘aging’). Together, UVB and UVA are equally responsible for causing sun cancers.
What about visible light? And blue light?
UV radiation is invisible to the human eye, but visible light from the sun is also problematic when it comes to melasma and more extensive pigmentation. Recent evidence shows that melasma pigment is exquisitely sensitive to blue-violet wavelength in the visible light spectrum. Blue light is the portion of the visible light spectrum with the shortest wavelength (400–495 nm) and greatest energy. It causes issues with pigmentation, but also causes redness, damaging Reactive Oxygen Species (ROS), and pro-inflammatory chemicals to increase in all skin types, especially darker skin tones.
When it comes to blue light from devices, studies show that you don’t need to be concerned about incidental light from devices, lamps, etc. The intensity of blue light emitted by these devices is much less than that emitted by the sun. However, masks or in-clinic treatments that contain LED lights emitting blue light at a very high intensity may drive pigmentation. If you’re being treated for pigmentation, it’s best to avoid these types of devices, or at least avoid the combined red-blue light modes on the device.
How do sunscreens protect against UV?
Chronic exposure to UVA and UVB rays lead to skin damage, premature aging, and skin cancer, as well as melasma and pigmentation. Sunscreens are designed to stop UV from reaching the skin (some also block visible light – more on that later).
SPF50 blocks 98% UVB, while SPF30 blocks 96%. It doesn’t seem like a big difference, but consider the UVB that actually gets through to the skin: SPF50 actually blocks twice as much as SPF30 (assuming you use enough of it!).
What about UVA? Well, the SPF number on your sunscreen only applies to UVB, because UVA has only recently been researched and found to be as big a problem as UVB. By law, the UVA protection must be at least 1/3 of UVB, but Australian regulations don’t require the UVA protection to be listed. Because of the 1/3 UVA/UVB equation, a higher SPF generally also means a higher UVA.
Is mineral sunscreen better than chemical?
The terms ‘mineral’ and ‘chemical’ refer to the types of UV filtering ingredients in sunscreen. Understanding the difference between them can help you make an informed decision about which one to use if you have melasma.
Mineral sunscreens contain inorganic or physical filters, such as zinc oxide (ZnO) or titanium dioxide (TiO2). Chemical sunscreens contain organic compounds, such as avobenzone, oxybenzone, or octinoxate, amongst many others. It’s important to note that all sunscreens, including mineral sunscreens, are technically chemicals.
Both types of sunscreens are effective in protecting your skin from UV, and both work the same way – by absorbing UV and converting it to a tiny amount of harmless heat. However, there are some differences between them that you should be aware of when choosing a sunscreen.
Firstly, mineral sunscreens tend to be thicker and heavier than chemical sunscreens, which can make them harder to apply and may leave a white cast on the skin. Chemical sunscreens are usually lighter in texture and easier to apply, and reapply multiple times during the day. Secondly, there is a common misconception that mineral sunscreens are safer or more ‘natural’ than chemical sunscreens. While it is true that mineral sunscreens can be derived from natural minerals, they are still processed in a lab with chemicals to remove any toxins before they can be used in skincare products. Any mineral makeup or sunscreen marketed into the USA, also must contain synthetic (lab-made) minerals by law, for safety and purity reasons (nothing ‘natural’ there!). And if a mineral sunscreen is marketed as ‘transparent’, those minerals are also made in a lab.
When it comes to melasma, you need a sunscreen that blocks both UVB and UVA, especially rays in the UVA1 wavelength. Zinc Oxide sunscreens are effective against UVA1, and many newer sunscreen chemicals are also excellent at blocking UVA1 radiation (and also don’t get absorbed into the skin like the older sunscreen filters).
Can you block blue light with sunscreen?
Well, yes, and no. When it comes to mineral sunscreens, one study showed that even a thick visible layer on the skin does not protect against blue light. The only known way to block blue light is by adding iron oxides to sunscreen. Iron oxides are the chemicals that produce a brown colour in cosmetics and tinted sunscreens. A concentration of >3% works best, which is why just wearing foundation over sunscreen isn’t enough. Many tinted sunscreens don’t contain the required amount of iron oxides, either.
Antioxidants like vitamin C and E can help reduce pro-inflammatory chemicals and damaging ROS from visible light exposure, but they don’t help with blue light protection if you’re concerned about pigmentation. This is because blue light interacts with melanosomes in the skin using a different mechanism than oxidation-induced damage.
What’s the take-home message?
So, if you have melasma, using proper sun protection, along with the right sunscreen (and using it correctly!) is crucial for the successful treatment and maintenance of pigmentation. The effectiveness of any sunscreen depends on how it is applied and how often it is reapplied. Regardless of whether you choose a mineral or chemical sunscreen, ensure it is heavily tinted, and apply the recommended amount of it to get the SPF protection stated on the container. And don’t forget to take other measures to protect your skin, such as wearing protective clothing, seeking shade, and staying inside during peak sun hours.
Our experienced dermatology nurse works with all Qr8 patients to create a simple, inexpensive and personalised skincare routine to support your treatment! This includes choosing the right sunscreen for your skin condition. Read more about how our melasma treatment works HERE.
REFERENCES
- Kaye ET, Levin JA, Blank IH, et al. Efficiency of opaque photoprotective agents in the visible light range. Arch Dermatol. 1991 Mar;127(3):351-5. PMID: 1998365.
- Cohen L, Brodsky MA, et al. Cutaneous Interaction with Visible Light: What Do We Know. J Am Acad Dermatol. 2020 Apr 11:S0190-9622(20)30551-X. PMID: 32289393.
- Lim HW, Kohli I, et al. Impact of visible light on skin health: The role of antioxidants and free radical quenchers in skin protection. J Am Acad Dermatol. 2022 Mar;86(3S):S27-S37. PMID: 34942294.
- Ruvolo E, Boothby-Shoemaker W, et al. Evaluation of efficacy of antioxidant-enriched sunscreen prodcuts against long wavelength ultraviolet A1 and visible light. Int J Cosmet Sci. 2022 Jun;44(3):394-402. PMID: 35587114.
- Geisler AN, Austin E, et al. Visible light. Part II: Photoprotection against visible and ultraviolet light. J Am Acad Dermatol. 2021 May;84(5):1233-1244. PMID: 33640513.
- Lyons AB, Trullas C, et al. Photoprotection beyond ultraviolet radiation: A review of tinted sunscreens. J Am Acad Dermatol. 2021 May;84(5):1393-1397. PMID: 32335182.
- Dumbuya H, Grimes PE, et al. Impact of Iron-Oxide Containing Formulations Against Visible Light-Induced Skin Pigmentation in Skin of Color Individuals. J Drugs Dermatol. 2020 Jul 1;19(7):712-717. PMID: 32726103.
- McDonald KA, Lytvyn Y, et al. Review on photoprotection: a clinician’s guide to the ingredients, characteristics, adverse effects, and disease-specific benefits of chemical and physical sunscreen compounds. Arch Dermatol Res. 2022 Nov 28. PMID: 36443500.
- Morgado-Carrasco D, Piquero-Casals J, et al. Melasma: The need for tailored photoprotection to improve clinical outcomes. Photodermatol Photoimmunol Photomed. 2022 Nov;38(6):515-521. PMID: 35229368.
- Duteil L, Cardot-Leccia N, et al. Differences in visible light-induced pigmentation according to wavelengths: a clinical and histological study in comparison with UVB exposure. Pigment Cell Melanoma Res. 2014 Sep;27(5):822-6. PMID: 24888214.
- Kohli I, Chaowattanapanit S, et al. Synergistic effects of long-wavelength ultraviolet A1 and visible light on pigmentation and erythema. Br J Dermatol. 2018 May;178(5):1173-1180. PMID: 28877342.
- Duteil L, Queille-Roussel C, et al. Short-term exposure to blue light emitted by electronic devices does not worsen melasma. J Am Acad Dermatol. 2020 Sep;83(3):913-914. PMID: 31887321.
- Soleymani T, Cohen DE, et al. Disparity in Cutaneous Pigmentary Response to LED vs Halogen Incandescent Visible Light: Results from a Single Center, Investigational Clinical Trial Determining a Minimal Pigmentary Visible Light Dose. J Drugs Dermatol. 2017 Nov 1;16(11):1105-1110. PMID: 29141058.
WOULD YOU LIKE TO CHAT TO ONE OF OUR FRIENDLY DOCTORS ABOUT YOUR SKIN CONDITION?
CLICK HERE TO BOOK A CONSULT WITH OUR EXPERIENCED MEDICAL TEAM.