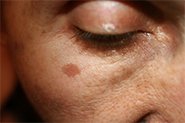
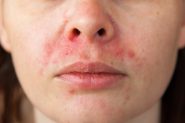
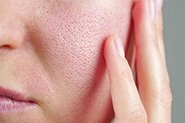
REAL PATIENTS. REAL RESULTS.






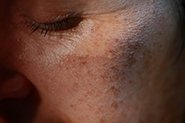
Amanda is using our day and night prescription creams that work together to target acne and scarring (post-inflammatory hyperpigmentation).
What Acne Is (And Isn’t!)
Acne (technical name: Acne vulgaris) is a common inflammatory skin disease that affects more than 80% of teens. But it isn’t limited to teenagers – adult acne can strike at any time, especially in females, even if you didn’t have teenage acne.
Acne is not a cosmetic condition – it is a medical skin disease. More specifically, a disease of the skin’s ‘pilosebaceous units’ – the hair follicle (that exits at the skin surface via a pore) and associated sebaceous gland that produces oil. Because it’s a medical condition, it is rarely fixed with complicated (and expensive!) skincare routines or cosmetic products and treatments. You need a targeted prescription acne treatment to manage it effectively.
There is no such thing as mild acne – all acne, even if it’s a single pimple or blocked pore, can and should be treated, especially if it makes you feel self-conscious or anxious. Acne and the dark marks it leaves behind (post-inflammatory hyperpigmentation, PIH) can make it difficult to attend school and work, socialise with friends, and generally enjoy life. And the best treatment for acne scars is to treat your acne effectively to prevent scar formation.
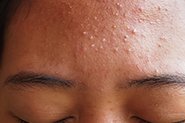
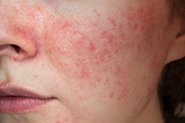
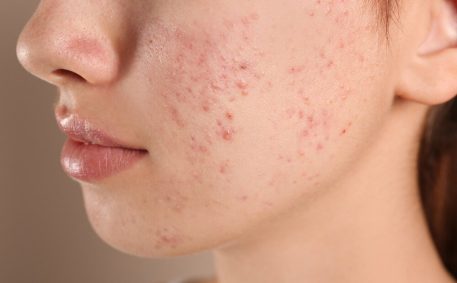
What Does Acne Look Like?
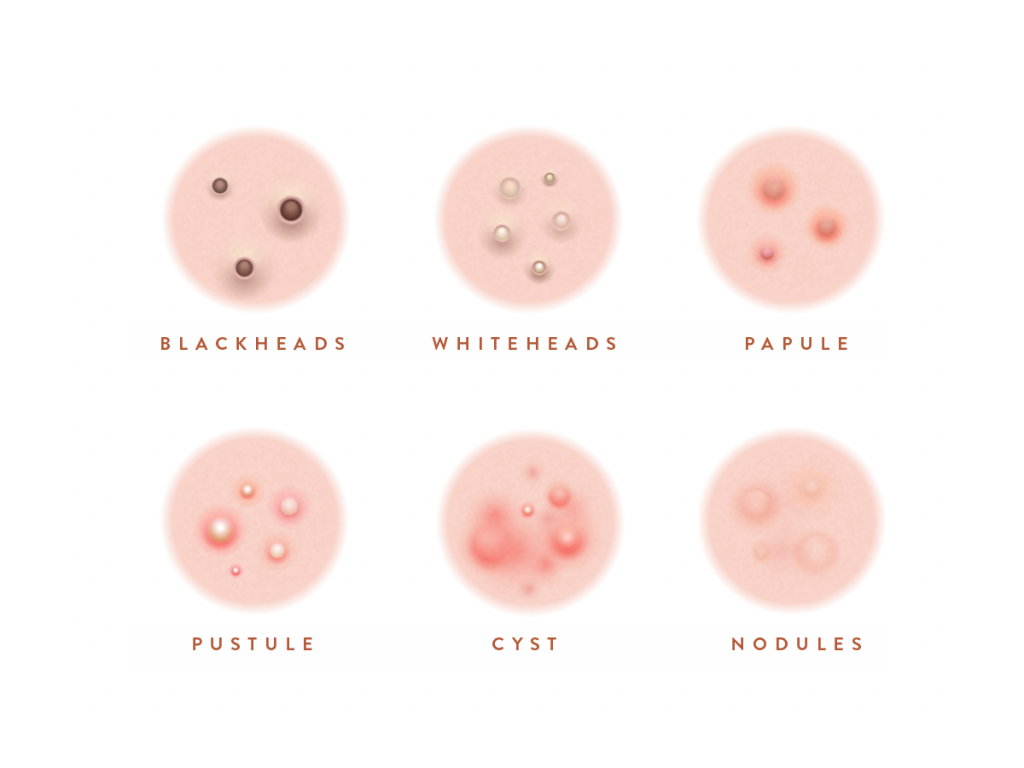
There’s no simple answer because acne lesions can be anything from clogged pores (also called comedones, which can be open (blackheads) or closed (whiteheads), papules (small red bumps on the skin) and pustules (like papules but filled with pus) to very large, painful, inflamed and swollen nodules and cysts (the dreaded ‘blind pimples’) – and sometimes all of these together! Redness, hyperpigmentation, scarring and pain are also common.
Read Dr Michele’s advice for dealing with the occasional blind pimple (cystic acne treatment), and the best acne spot treatments in Marie Claire Australia HERE
What Causes Acne?
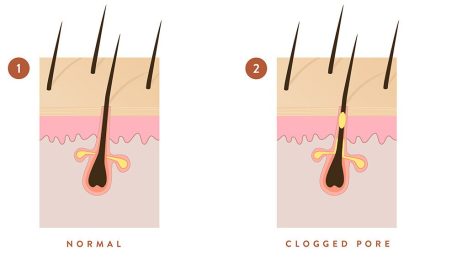
It all starts with a clogged pore. Acne sufferers produce excess oil (‘sebum’) and the skin cells lining their pores don’t shed properly, instead collecting in the pore. The sticky skin cells and oil mix together in the pore, creating a microscopic blockage called a microcomedone.
Acne bacteria (Cutibacterium acnes, which used to be called Propionibacterium acnes) feed on sebum, gathering in large numbers around this oily plug, signalling the body to start producing chemicals that ramp up inflammation.
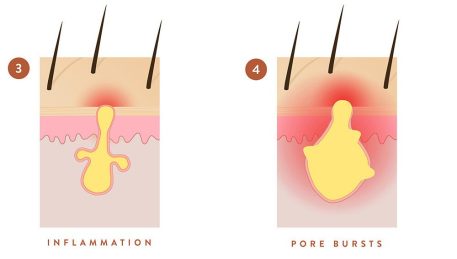
The inflamed plug gradually enlarges to form a visible comedone.
Eventually the pore bursts and bacteria and oil leak into the surrounding tissue, creating even more inflammation, and causing other acne lesions like papules, pustules, nodules and cysts.
Which Hormones Cause Acne?
Excess sebum production (‘seborrhoea’) is driven by hormones. The hormones involved are called ‘androgens’, and include dihydrotestosterone (DHT) and testosterone.
Both males and females produce androgens, either in their adrenal glands, testes or ovaries or converted from precursor chemicals in the skin, hair follicles, sweat glands and sebaceous glands. Circulating androgens bind to receptors on oil glands and stimulate them to produce excess sebum, creating the perfect conditions for acne formation
Teenage acne is common due to the natural increase in androgen hormones during puberty, but adult acne is more common than you think – it can flare during menstruation (it’s thought that this is because less oestrogen is available to suppress androgens), and pregnancy. So adult acne treatments are also important.
Because of its hormonal basis, dermatology treatments for acne can include anti-androgen drugs such as oral contraceptives, spironolactone and cyproterone acetate (Androcur). Vitamin A can also reduce sebaceous gland activity.
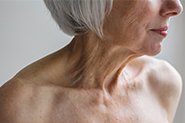
Don’t Forget Chest And Back Acne (‘Backne’)
Acne doesn’t just affect your face – it can appear on your chest and back (and sometimes your upper arms) as these areas have loads of sebaceous glands.
What Doesn’t Cause Acne?
Acne isn’t caused by a lack of hygiene or ‘dirty’ skin – so no amount of cleansing, scrubbing or exfoliating will get rid of it. In fact, this can inflame skin and make everything worse! Acne is simply a medical condition, that needs a medical solution.
Read more about some common acne myths HERE.
Can I Fix My Acne With Diet?
There is still no conclusive scientific evidence to suggest that diet causes acne. High-glycaemic foods and dairy can trigger breakouts for some (but not all!) people who are already predisposed to acne. Read more about skin health & acne HERE. If you’re going to seek advice about diet and acne, make sure it’s evidence-based advice from an Accredited Practicing Dietitian.
And ignore advice from ‘experts’ on social media trying to sell you supplements – they don’t work!
Remember that you just have a medical skin condition that can be managed with simple medical treatment – you’re not doing anything wrong!
What is post-inflammatory hyperpigmentation (PIH)?
PIH is a reaction to injury or inflammation that causes the skin to produce increased melanin pigment. It is more common in those with deeper skin tones. The most common cause of PIH is pimples, but it also can result from inflammatory skin conditions, burns, a reaction to skincare products, medications, or treatments, or any skin injury (like picking at zits!).
PIH appears as dark spots/patches in the same area as the healed injury. These marks can take several months or years to resolve – up to 5 years in some cases. PIH can get darker and persist in the skin for longer when exposed to sunlight (so don’t forget your sunscreen!).
Our doctors can customize a treatment cream to fade PIH at the same time you are treating your acne breakouts. You can discuss this during your 1:1 video consult with our experienced doctors
WHAT’S THE BEST PRESCRIPTION ANTI-ACNE TREATMENT FOR TEENAGERS AND ADULTS?
There are loads of over-the-counter acne cleansers and acne treatment skincare aimed at unclogging pores (salicylic acid, glycolic acid) and killing bacteria (benzoyl peroxide, which also has a pore unclogging effect). These often don’t fully clear breakouts. This is because they don’t target all the factors that cause acne – oil, sticky skin cells, bacteria and inflammation.
That’s where Qr8 MediSkin comes in! Our doctors can customise the best acne treatment product for you – one that targets all the acne-causing pathways to help you manage acne (and post-inflammatory hyperpigmentation at the same time). Without the need to visit an acne dermatologist, or wait in line at the pharmacy.
But we don’t just give you access to the best customised acne skin treatments. We are the Australia’s go-to service for support so you can use your acne product safely and effectively to get results:

We get to know you – We ask about triggers like hormonal influences, and how your breakouts affect how you feel, so our doctors can invest time during your 1:1 video consult helping you get the most from your acne treatment.

Our Skincare Support Team provides advice and support to all our patients, including access to our specialist guides on how to minimise retinization (irritation, peeling and redness) and purging (temporarily getting more pimples before your acne clears) that can sometimes happen when you start treatment. We also help you find the best sunscreen to prevent those PIH dark spots sticking around.
We design the best acne treatment for you – Our doctors use clinical guidelines developed by our in-house medical and scientific team, based on the most current and best-available evidence. They use these to design the best acne treatment for you – a skin treatment cream for acne with a fully customised blend of active ingredients that can be adjusted to suit your skin’s tolerance, allergies and sensitivity level, available only on prescription.
Your Customised Prescription Acne Treatment Medication
Our treatments include a combination of acne-busting ingredients designed just for you:
We even have pregnancy-safe options to tackle pregnancy breakouts!
Why We Don’t Use Antibiotics In Our Skin Treatments For Acne
Although antibiotics can be successfully used in acne treatment creams, common anti-acne antibiotics like clindamycin and erythromycin result in high rates of antibiotic resistance in acne bacteria (without also using something like benzoyl peroxide for example). Antibiotic-resistant acne bacteria can also persist on your skin long after you finish using the antibiotic cream. And having antibiotic-resistant bacteria on your face means your acne treatment can be less effective. The resistant bacteria can also be transferred to close contacts!
Instead of topical antibiotics, our doctors use prescription-strength azelaic acid (15%-20%) if required to kill acne bacteria. Azelaic acid isn’t an antibiotic (so resistance has not been reported) but research shows that 20% Azelaic acid applied twice daily for 12 weeks is comparable to 1% topical clindamycin + benzoyl peroxide in reducing acne lesions. And it’s good news if you’re pregnant – Azelaic acid is a pregnancy class B drug (no evidence of risk in studies).
Sometimes, our doctors may recommend a very short course of oral antibiotics in combination with a topical retinoid. Our doctors choose antibiotics known to result in the lowest rate of antibiotic resistance in acne patients, and they will only be used if absolutely necessary
DO I NEED TO WORRY ABOUT SKINCARE BLOCKING MY PORES?
Comedogenicity (the potential of a formulation clog pores and cause blackheads/comedones) is an unreliable science. The method used to test a product’s comedogenicity rating (on a scale from 0-5, with 5 being most likely to block pores and therefore cause acne) involves test subjects placing the product on their back skin for 48-72 hours, multiple times over 4 weeks.
A skincare product label might be labelled as ‘non-comedogenic’ but this is nothing more than marketing jargon. Here’s why…
Back skin isn’t the same as facial skin, so something can be comedogenic in the test, but not cause any issues on facial skin.
An ingredient can be comedogenic when used in a high concentration in tests, but when used in a lower percentage in a cosmetic product, is not comedogenic.
The term ‘comedogenic’ and the comedogenicity rating scale is not regulated by any governing body, so it can mean anything, and is therefore meaningless!
The good news is that you don’t need to worry! When you are using the best medical treatment for your acne, it will override any potentially comedogenic ingredients in your skincare. Our Skincare Support Team can help you choose the best skincare for acne to ensure your skin stays comfortable whilst you use your acne treatment cream.
Read more about comedogenic skincare and other beauty marketing jargon HERE.
Listen as one of our clients discusses how our service works (and the best skin treatment for acne) HERE
Do I need to spend a lot of money on skincare to support my acne product?
Click HERE to read what our founder, Dr Michele Squire, told Mamamia Australia about expensive skincare (all our patients receive personalized 1:1 advice from our Skincare Support Team about inexpensive skincare products to support their acne treatment product. It’s part of our all-inclusive cost – read more in our FAQ.
Retinoids and Acne
We discussed this with dermatologist, Dr Natalia Spierings in our Instagram Live Skin Sessions Series. Click HERE to watch.
Acne Medications And Purging
Purging is one of the possible initial side effects of prescription retinoid use, especially if you had a lot of comedones (bumps under the skin) to start with. What you will also have, but can’t see, are ‘microcomedones’ – pores that were already blocked, but invisible to the eye.
Retinoids speed up the shedding of skin cells to regulate the sticky skin cells that block your pores and lead to pimples. Unfortunately, in the initial stages of treatment, at the same time as treating your acne, you are also temporarily blocking pores with extra skin cells, pushing existing comedones to the surface, and causing microcomedones to turn into ‘actual’ comedones.
So the pimples that might have surfaced over the next few months can all appear at once!
If you are one of the unlucky few that this happens to, it is definitely NOT fun. If you already suffer from acne, it will feel like your treatment is making things worse, not better.
The good news is, that as you continue to use your retinoid and these blockages are pushed to the surface and clear, you can expect fewer new breakouts. The other good news is that purging gets a lot more air time on social media than it occurs in real life, so it may not even happen for you!
Our service includes a range of written guides, based on the most up-to-date scientific evidence, to help you manage side effects like acne purging. You also receive full access to 1:1 personalized support from our experienced Skincare Support Team. This is included in the one-off, all-inclusive cost of your treatment.
References