Our Clinical Director, Dr Scott Ellis, answers the burning questions about mask acne (maskne)…
Is maskne (mask acne) something new that arrived with COVID-19?
The term ‘maskne’ is relatively new, but the medical skin condition that it refers to (called ‘acne mechanica’) is not.
First described in the scientific literature in 1975[1], acne mechanica is something that traditionally is most commonly seen in soldiers and athletes wearing tight-fitting protective equipment. The friction, heat and lack of breathability of their protective equipment (such as helmets, chin straps and shoulder pads) causes a dermatological condition that looks identical to common acne, but has different underlying causes. Since it was first described there has been little interest in studying and understanding the disease, but this has changed recently with the sharp increase in case numbers caused by prolonged mask-wearing.
How can face masks cause acne? Is it different to regular acne?
When wearing a mask for long periods of time on a regular basis, our facial skin is exposed to 3 main factors that cause maskne – increased relative humidity, increased temperature and mechanical friction.
Increased relative humidity: The air we breathe out creates high humidity under our masks, resulting in the overgrowth of certain bacteria & fungi that live on our skin – we call this microbiome imbalance[2]. Additionally, the increased humidity causes the surface cells of the skin to absorb more water and swell, creating blockages at the surfaces of our pores[3].
Increased temperature: Decreased air circulation traps heat, raising the surface temperature of our skin. As a result we see increased oil (sebum) production, with small increases in temperature able to create significant increases – an rise of just 1 degree celsius can increase sebum production by 10%[4]. The sebum becomes trapped in the skin because of the blocked pores, and promotes the development of inflammation & acne.
Rubbing & friction: Compounding the developing inflammation in the skin, areas where the mask rubs on our skin disrupts the protective skin barrier and further creates swelling & inflammation[5]. This feeds into the cycle created by the humidity & temperature increases, worsening the situation.
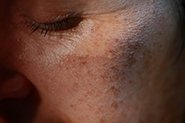
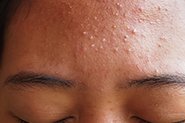
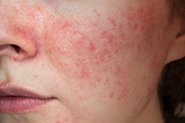
The overall result is the development of red bumps (papules), blackheads/whiteheads (open & closed comedones), and pimples (pustules) that are typical of acne mechanica. It’s important to note, however, that these changes can also be seen in other diseases that may be worsened by masks[6] – such as rosacea, perioral dermatitis or malassezia folliculitis (overgrowth of fungi in the hair follicle).
How can you tell whether your acne is caused by mask wearing or something else?
In some instances it is fairly easy to tell if your acne issues are caused by mask wearing. Dead giveaways include:
your breakouts are only occurring in areas that are covered by your mask
breakouts tend to be worst in areas that see the most friction from your mask (such as the bridge of the nose, or prominent areas of the cheek)
the condition of your skin improves if you’re able to not wear your mask for a few days (e.g. over the weekend, or if you’re working from home).
Other times it can be quite difficult to figure out whether your acne is caused by your mask, if your skin is showing signs of an allergic reaction to something (what we call an acneiform eruption) or if your symptoms are being caused by another medical condition with a similar appearance[6] (such as rosacea or perioral dermatitis mentioned above).
The best way to figure this out is to consult with a doctor about your issues – ideally one who specialises in treating skin, as most practitioners don’t see or treat acne mechanica in their daily practice.
How do you treat maskne? Do I need to buy new skincare products to treat it?
The most effective ways to treat acne mechanica are quite simple, but important:
Change your mask regularly: Masks are undeniably important in helping manage the impact of COVID, but that doesn’t mean we can’t look at ways to safely improve the situation for our skin. If it’s safe to do so, put aside a little bit of time in your day to change to a fresh mask and let your skin take a short break. 10-15mins should be long enough to help decrease the effects of the mask microclimate and provide your skin some respite. If you have very oily skin, you may wish to wipe away excess surface sebum with micellar water or a gentle face wipe. Avoid wipes with fragrance or essential oils, as these can be irritating. Switching to a fresh mask will decrease the humidity and keep the skin clean, and have the added bonus of being more effective (all masks lose some of their effectiveness as they absorb moisture). If using cloth masks, be sure to wash them after every wear – putting used masks back on is not only bad for infection control, but is also bad for your skin. Wash your masks with a shampoo made for sensitive skin rather than washing detergent, as any residual detergent left on your mask may cause irritation or a contact dermatitis.
Skip the makeup: Your skin is already struggling with congestion under your mask, so skip using makeup in the covered area if possible. It’ll decrease your risk of skin congestion and irritation – and nobody can see through your mask anyway!
Simplify your skincare: Traditionally, signs of acne cause many of us to reach for ingredients that can be helpful to manage acne of other causes – such as alpha-hydroxy acids (glycolic acid), beta-hydroxy acid (salicylic acid), benzoyl peroxide or aggressive cleansers. In Australia it’s not uncommon for these products to be overused at the best of times – even though people are trying to do the best for their skin, much of the time they are unknowingly stripping it and causing more inflammation by impairing their skin barrier (if your skin feels tight after cleansing, or you’re having to use multiple hydrating and moisturising products every day then this may be you!). One of the main issues in acne mechanica is impairment of the skin barrier – so taking the same approach and using a combination of these ingredients is likely to make your maskne worse. For most people the best approach is to simplify back your skincare to a gentle cleanser appropriate for your skin type, a high-quality sunscreen and a simple, non-fragranced moisturiser (CeraVe, QV or La Roche-Posay Toleriane are some of my favoured moisturiser recommendations).
Seek advice if you’re still struggling: If you’re still having difficulty despite the above approaches, it’s best to speak to your doctor. Not all acne is the same – everyone’s skin physiology and causative factors are different, and in some cases, it’s not even acne! It still amazes me how often people are recommended products or a skincare regime without being asked any questions about their skin or acne. A certain ingredient, regime or treatment approach might help some people, but without first understanding the causative factors for your specific skin concerns it’s impossible to create a treatment plan that will create the best possible results. A good practitioner will explore your concerns, ask detailed questions regarding your skin and look at your skin closely to help accurately diagnose your issues and put together an evidence-based treatment plan to help. For acne mechanica this may involve creams with medications such as azelaic acid and prescription retinoids, or in more severe cases oral medications may be used to help settle your skin. The key is to seek advice and treatment early in order to get the best results and minimise any risk of skin scarring.
Does wearing a silk (or other material) face mask help prevent maskne?
There’s lots of marketing surrounding silk products such as face masks and pillowcases for acne and other skin conditions. The reality is that there are no medical studies that support the claim that silk masks help to prevent acne mechanica, acne vulgaris (regular acne) or any other dermatological disease.
There is some early laboratory data that suggests that silk has an advantage over other cloth materials (such as cotton or polyester) in that it absorbs less water, meaning that it can be worn again sooner after washing and may repel aerosolized water droplets more effectively[7] – however there are no clinical studies that have been performed to measure this and as such there is no scientific basis to favour silk masks at this stage. As with all cloth masks, their efficiency is far less than those of purpose-built medical disposable masks[8].
For more information about how we treat regular acne (acne vulgaris) CLICK HERE
REFERENCES
WOULD YOU LIKE TO CHAT TO ONE OF OUR FRIENDLY DOCTORS ABOUT YOUR SKIN CONDITION?
CLICK HERE TO BOOK A CONSULT WITH OUR EXPERIENCED MEDICAL TEAM.