Skin rashes can be difficult to tell apart at the best of times, even for doctors. In some cases, it’s not all that important to get an exact diagnosis, as many rashes are treated with the same medications. This couldn’t be further from the truth for periorificial dermatitis (PD), as it mimics other skin presentations such as acne & eczema – and quickly spirals out of control when the wrong treatment is prescribed. In fact, many of the treatments for other rashes cause periorificial dermatitis to become worse, leading to long periods of discomfort and an unsightly rash.
Let’s look at the basics of PD to get an understanding of how it differs to other diagnoses and why we have to approach treatment differently.
What is PD?
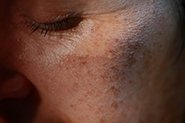
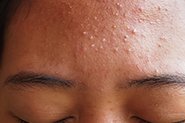
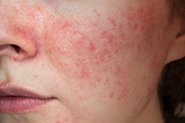
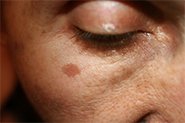
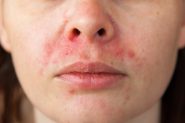
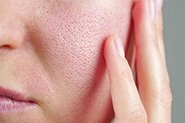
Periorificial dermatitis is relatively common, with an estimated 1 in 100 people experiencing an episode each year. The rash is fairly unique – usually made up of groups of itchy or tender small red lumps (papules) overlying irritated skin, following typical patterns on the face. Often, it’s accompanied by skin barrier dysfunction, demonstrated by burning or tingling with application of even the blandest skincare, and with time may also develop tiny pustules that look like clumps of small pimples.
We call it ‘periorificial’ as it develops around the mouth, nostrils and/or eyes – referred to as perioral, perialar or periocular dermatitis when occurring in one area alone (although the disease process is the same). It usually spares the cheeks, forehead and skin immediately surrounding the lips, creating a tell-tale pattern of normal skin areas.
While we understand the patterns that occur, unfortunately we don’t yet fully understand why it occurs. Current evidence suggests that a number of factors contribute including skin barrier dysfunction, the innate immune system (our body’s first-line immunological defence), imbalanced microflora of the skin, hormonal fluctuations and reactions to things we put on the skin such as steroid creams, makeup ingredients, skincare ingredients and sunscreens.
Why is accurate diagnosis important?
Due to the varied appearance of PD we commonly consult people who have been misdiagnosed with contact dermatitis, eczema, acne, rosacea and seborrheic dermatitis. This creates a problem – as the common treatments for these conditions often worsen PD. Steroid creams, for example, generally make the rash look less angry for a few days, but cause it to flare much worse when the steroid is removed. Sometimes this cycle is repeated multiple times before we consult someone, meaning that the dermatitis is severe before someone begins down the road of appropriate treatment.
What can be done to treat it?
In general, the best way to treat PD is with a ‘less is more’ approach. Stripping back skincare to a simple, bland supportive regimen is the first step, being sure to identify and exclude any products that may be driving inflammation (those with essential oils, fragrances, daily or high strength exfoliants, long ingredient lists with lots of actives, and sometimes even prescription retinoids, are often problematic). Good barrier support is a must, with personalised recommendations made depending on the state of your skin. For some, this approach over time is enough to settle the dermatitis.
Depending on how severe your PD is, your doctor may also choose to start you on a cream, oral antibiotic or a combination of both. Immune modulating medications commonly selected include metronidazole, pimecrolimus or tacrolimus, which are aimed at decreasing the inflammation and over-activity of the innate immune system in the skin. Your doctor chooses the treatment agent(s) depending on your health and skin condition overall. A sub-antimicrobial oral antibiotic is generally selected when needed, significantly decreasing the risk of antibiotic resistance in your body.
Why is it important to treat it early?
Periorificial dermatitis can be stubborn, and treatment generally takes time. In some instances, the most effective management for perioral dermatitis can require 3-4 months of ongoing treatment, even beyond the time that symptoms disappear in order to prevent recurrence. In general, the earlier the correct treatment is commenced for PD, the quicker we achieve resolution.
In short, PD can be tricky to diagnose & manage. If this all makes your head spin, don’t worry – the most important part of perioral dermatitis treatment is ensuring that you’re getting diagnosed accurately, treated quickly and have ongoing support and detailed advice on hand for when you need it.
Periorificial dermatitis can get out of control quickly. CLICK HERE to see what this looks like!
REFERENCES
Shadfar S, Perkins SW. Anatomy and physiology of the aging neck. Facial Plast Surg Clin North Am. 2014. PMID: 24745379.
Tempark T, Shwayder TA. Perioral dermatitis: a review of the condition with special attention to treatment options. Am J Clin Dermatol. 2014. PMID: 24623018.
Balić A, Vlašić D, Mokos M, Marinović B. The Role of the Skin Barrier in Periorificial Dermatitis. Acta Dermatovenerol Croat. 2019. PMID: 31542061.
Ollech A, Yousif R, et al. Topical calcineurin inhibitors for pediatric periorificial dermatitis. J Am Acad Dermatol. 2020. PMID: 32032693.
Tolaymat L, Hall MR. Perioral Dermatitis. 2021 Sep 13. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2021 Jan. PMID: 30247843.
Lee H, Kim KH. Treatment of pediatric periorificial dermatitis with topical calcineurin inhibitor and topical/oral metronidazole. J Dermatol. 2021. PMID: 33275294.
WOULD YOU LIKE TO CHAT TO ONE OF OUR FRIENDLY DOCTORS ABOUT YOUR PERIORIFICIAL DERMATITIS?
CLICK HERE TO BOOK A CONSULT WITH OUR EXPERIENCED MEDICAL TEAM.