What is Keratosis Pilaris?
Keratosis Pilaris (KP) is a very common, but harmless, skin condition that can run in families. It is more common in children, teenagers and those with dry skin or eczema. It affects 50–80% of adolescents and up to 40% of adults, worldwide. Unfortunately, it is also a chronic skin condition that needs consistent management, although some people do grow out of it with age (typically after age 16).
What causes it?
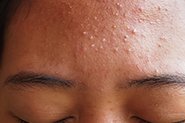
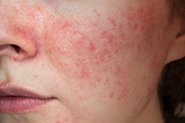
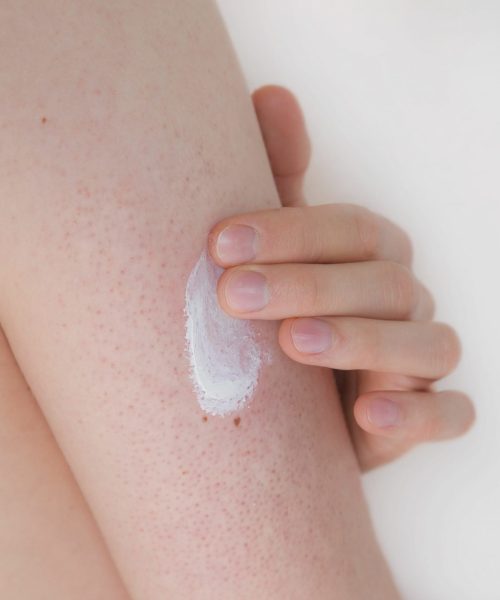
KP appears as tiny white or skin coloured bumps that look similar to goose bumps, making the skin feel rough or ‘sandpapery’ to the touch, and can be itchy at times. In those with lighter skin tones, the skin surrounding the bumps can also appear red. KP typically appears on the skin of the upper outer arms and the front of thighs, although it can extend to the buttocks and facial cheeks (especially in young children). KP bumps are sometimes mistaken for pimples, but they are actually plugs of dead skin caused when excess keratin (skin protein) gets trapped in the hair follicle, along with a coiled up hair – as shown in the diagram below:
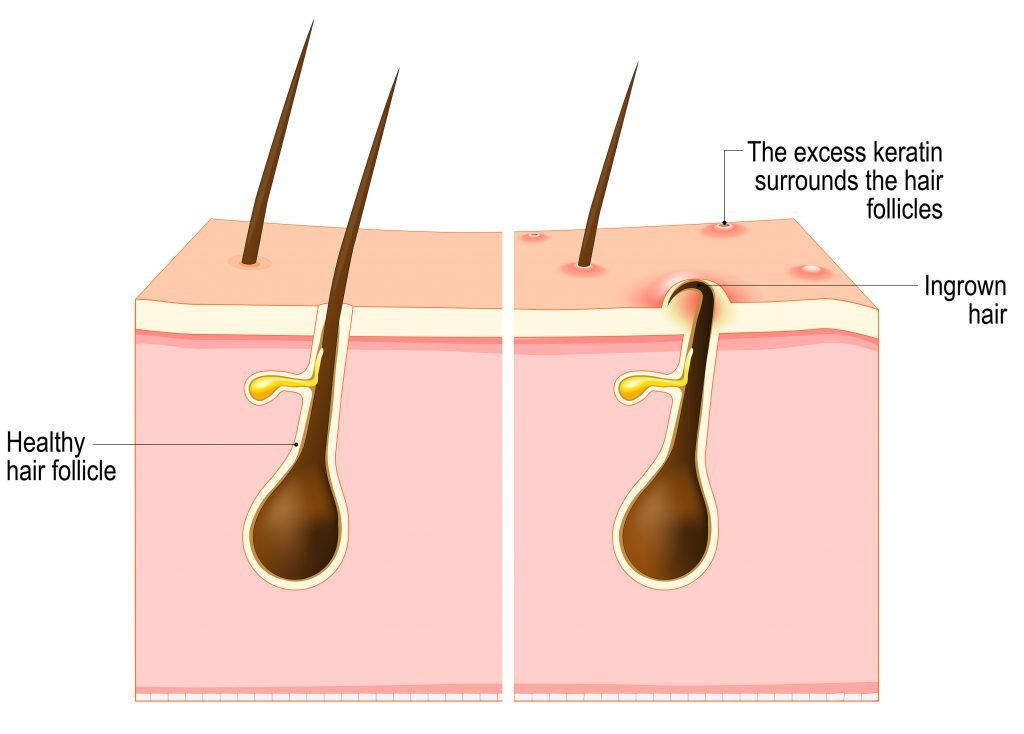
KP usually becomes more noticeable during winter due to lower humidity and friction from heavier winter clothing. Although harmless, the appearance and feel of KP bothers many people, so they seek treatment before exposing their skin in the warmer months. If it doesn’t bother you, you don’t need to treat it.
How can I get rid of KP?
Unfortunately, there is no cure for KP, but it IS manageable.
Preventing dryness and itching is the first step (not scrubbing and exfoliating, which is where most people start!). Just use a gentle, non-fragranced skin cleanser, avoid long hot showers/baths, and apply a rich, fragrance-free moisturiser twice daily whilst skin is damp, straight out of the bath or shower (plain petroleum jelly has the best evidence for improving KP severity, but make sure you only use a tiny amount and rub it in well if you don’t want to ruin your clothing/bedding). If your skin feels itchy during the day, apply more moisturiser.
Adding a humidifier to your bedroom or office space during winter can also help.
And if you really MUST exfoliate – make sure it’s super gentle, and you always apply a moisturiser afterwards.
What kind of moisturiser is best?
Moisturisers containing keratolytic ingredients that break down the keratin plug (such as urea >10%, lactic and salicylic acids) and help gently unblock the follicles are very effective, whilst still being gentle.
We recommend the CeraVe SA smoothing Cream. Massage this into the affected areas after every bath/shower, or at least twice daily.
What if this doesn’t work?
If these DIY techniques don’t have any effect after 6 weeks, or if there is a lot of redness, it’s time consult a doctor for advice.
Topical azelaic acid, tacrolimus, the prescription retinoid tazarotene (not tretinoin), and/or low-potency steroid cream are all evidence-based treatments that can be prescribed to help (paired with the skin-softening treatment outlined above). But, compounded creams can be expensive when used over an extensive skin area, and there may be a short-term increase in redness as the skin adjusts to treatment (so it’s worth doing it in winter).
If all else fails, there is early evidence that QS Nd: YAG laser treatments may be effective, but use with caution for those with skin of colour, as post-inflammatory hyperpigmentation can occur.
Are you a current Qr8 MediSkin patient? Access our Patient Library, where you can find lots more evidence-based information about skin topics, CLICK HERE.
REFERENCES
- Maghfour J, Ly S, et al. 2022. Treatment of keratosis pilaris and its variants: a systematic review. J Dermatolog Treat. PMID: 32886029.
- Kechichian E, Jabbour S, et al. 2020. Light and laser treatments for keratosis pilaris: A systematic review. Dermatol Surg. PMID: 32804891.
- Hwang S, Schwartz RA. 2008. Keratosis pilaris: a common follicular hyperkeratosis. Cutis. PMID: 18856156.
WOULD YOU LIKE TO CHAT TO ONE OF OUR FRIENDLY DOCTORS ABOUT YOUR SKIN?
CLICK HERE TO BOOK A CONSULT WITH OUR EXPERIENCED MEDICAL TEAM.